When deciding on having bariatric surgery, there are certainly many decisions to be made. If you choose to have a laparoscopic sleeve gastrectomy (LSG), one consideration may be the potential side effects. Mayo Clinic states that during the LSG, or vertical sleeve gastrectomy, “about 80% of the stomach is removed, leaving a tube-shaped stomach about the size and shape of a banana.” This procedure limits the size of the stomach, which decreases the amount of food you can consume, while also leading to hormonal changes which can aid in weight loss. While Annals of Medicine and Surgery states that the LSG is the most common bariatric surgery performed, it’s not without its potential complications.
What is a gastric sleeve leak?
When you have an LSG, New York Bariatric Group reports, your surgeon will use staples to seal the stomach after removing the 75-80% in order to create the sleeved shaped stomach. It’s at this staple line where leaks would occur after surgery.
If the staples come apart, or if your body doesn’t heal correctly and form a complete seal, contents and gastric juices from the gastrointestinal (GI) tract can leak through. This is problematic, as this fluid contains bacteria and, if it leaks into the abdomen, can cause infection.
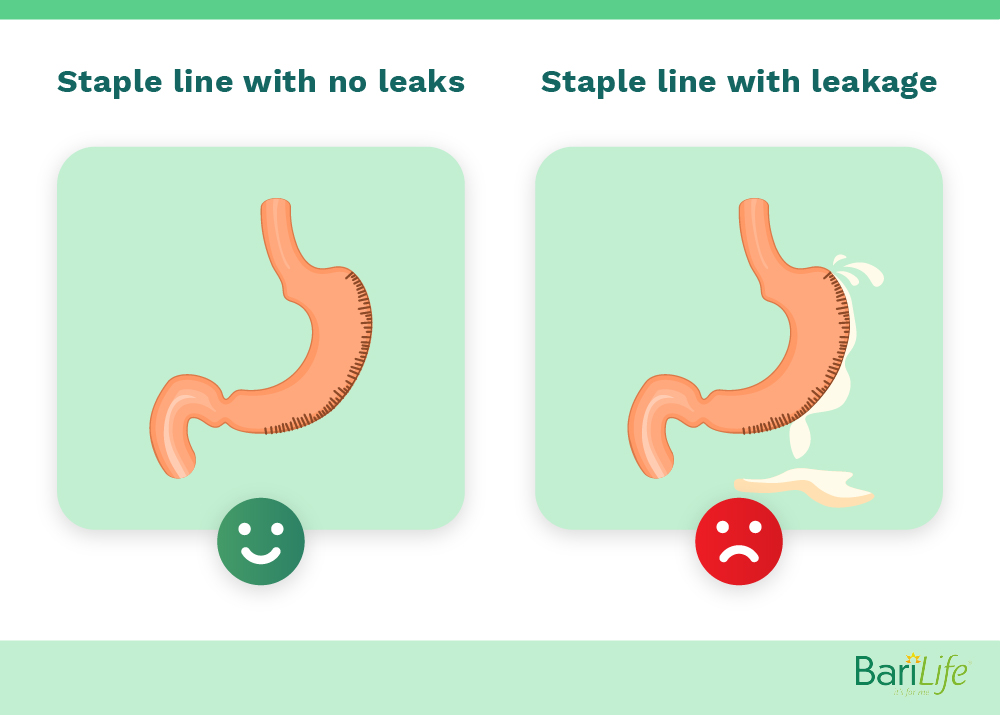
In a study published by the Alexandria Journal of Medicine, the highest percentage of leaks were seen in those individuals who had an LSG. 70% of patients who had a leak had the leak at the staple line just below the esophagogastric junction (where the esophagus meets the top of the stomach), which is the most commonly reported leakage site.
What are the signs and symptoms of a gastric sleeve leak?
The Alexandria Journal of Medicine study noted that leaks after bariatric surgery are difficult to diagnose, and do come with increased morbidity and mortality. In this study, the average time for diagnosis of a leak was 3.9 + 2.6 days. Signs and symptoms noted in this study included tachycardia (elevated heart rate), fever, tachypnea (rapid breathing), left shoulder pain, abdominal pain, chest pain, oliguria (producing less urine), and/or hypotension (low blood pressure).
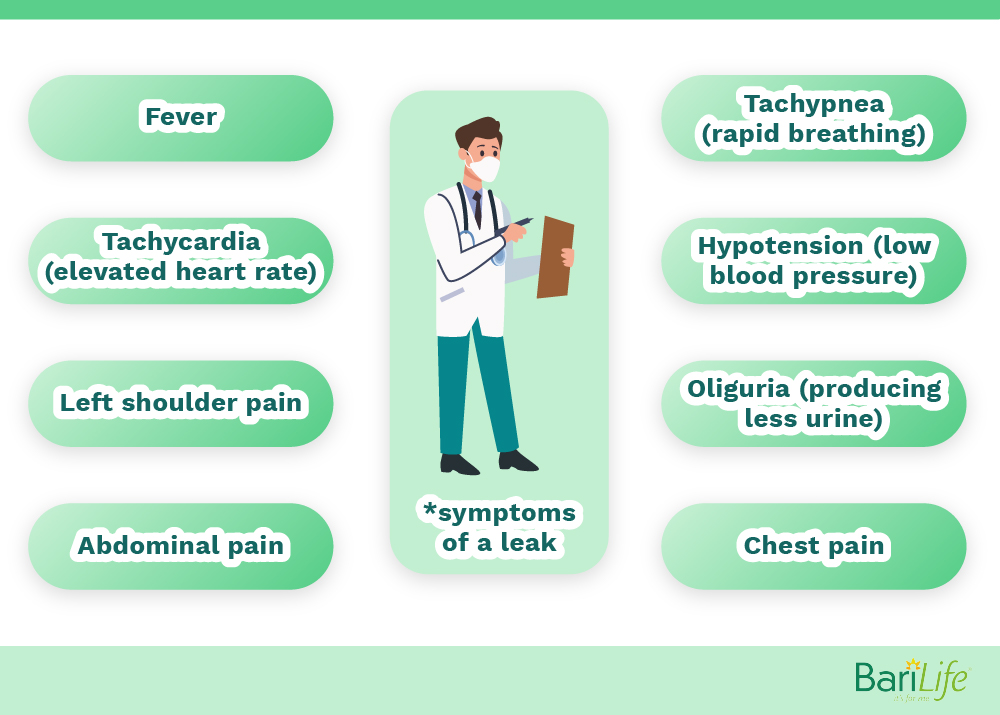
I think I may be having some of these symptoms…how does a doctor diagnose a leak?
In order to diagnose a leak after bariatric surgery, doctors can use Gastrografin. Per NPS MedicineWise, Gastrografin is a liquid that is swallowed, which acts as a dye during an X-ray. A doctor can ask the patient to swallow the liquid, and then will take an X-ray of the patient’s GI tract. As the Gastrografin flows through, it will allow the radiologist to see what’s going on in the GI tract more clearly on the X-ray, which can help them to identify if you’re having a gastric leak.
How common are these leaks?
In the study we discussed earlier from the Alexandria Journal of Medicine, they found that 1.6% of patients who underwent bariatric surgery had a leak. Something to note here is that this study included multiple different types of bariatric procedures, including LSG, laparoscopic gastric bypass (LGB), and open gastric bypass. When looking at those patients who had the LSG specifically, they found that 6.3% of these patients had a leak. Of note, leaks were the most common in patients who had the LSG, as opposed to other bariatric procedures. The study suggests that the increased incidence of leaks in patients who receive the LSG procedure may be due to higher pressure in the gastric pouch.
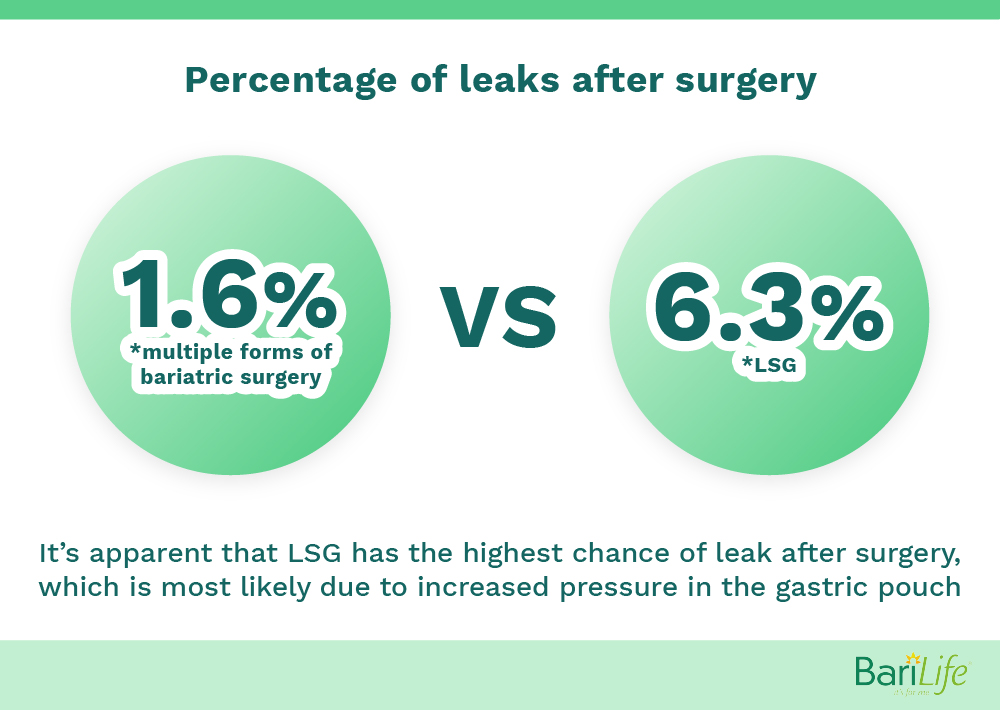
A different study in the World Journal of Gastrointestinal Surgery found that 1.2% of patients in their study who had the LSG were found to have a leak. While studies may differ slightly in the data, a review published in the World Journal of Gastrointestinal Surgery notes that the leak rate can vary between 1-3% of patients during their first sleeve gastrectomy.
What if I have revision surgery?
Advanced Surgeons – Westchester Bariatric & Weight Loss Surgery notes that the American Society for Metabolic and Bariatric Surgery (ASMBS) classifies revision surgeries into three different categories: conversion, corrective, and reversal. A conversion surgery involves changing the original bariatric procedure into a different one, such as converting an adjustable gastric band to a sleeve gastrectomy. A corrective surgery modifies the original surgery, in an effort to make it more effective or to fix an issue. Finally, a reversal procedure restores the original gastric anatomy.
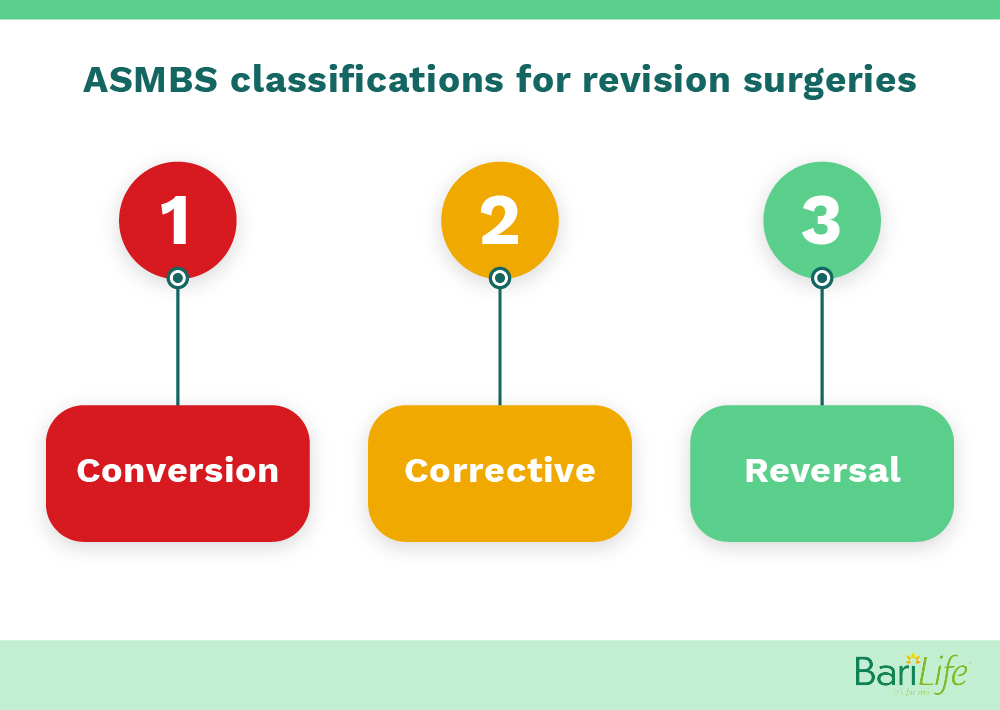
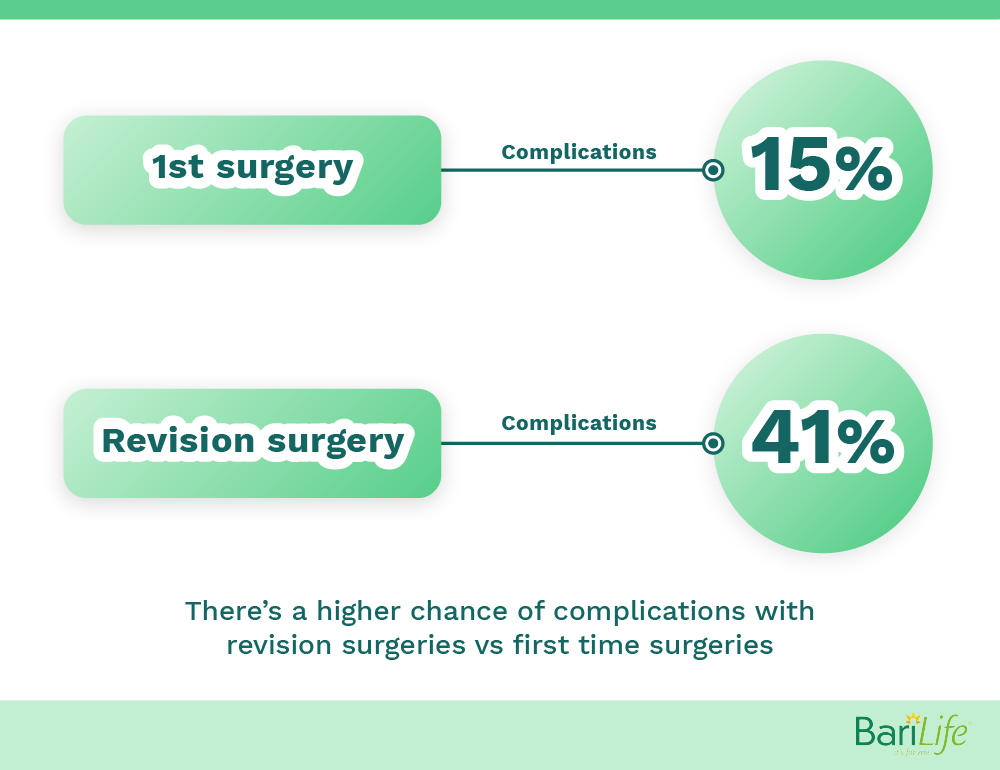
If you have revision surgery, the Canadian Journal of Surgery notes, you’re unfortunately more likely to experience complications. In their study, 41% of patients who had a revision surgery experienced some sort of complication, as compared with 15% of patients who were having their first bariatric surgery. Again, it’s important to note here that this study included patients who were having multiple types of gastric bypass surgeries, not just an LSG.
Unfortunately, with increased risk of all complications comes increased risk of a leak specifically. The Trauma Surgery and Acute Care Open journal published a study in which it found that leaks were more common in revision surgeries. In their study, 18% of patients who had a revision surgery experienced a leak. Overall, the World Journal of Gastroenterology found that >10% of patients who have a revision surgery suffer from a gastric leak.
Nonsurgical treatment options
Depending on the severity of the leak, the World Journal of Gastroenterology notes that it may be treated either surgically or nonsurgical. The American Society for Metabolic and Bariatric Surgery (ASMBS) notes that nonoperative management may be appropriate for patients who are more clinically stable. The doctor can take an Upper GI series, which is a set of images that allows them to see what’s happening inside your GI tract in order to determine the location of the leak and the severity.
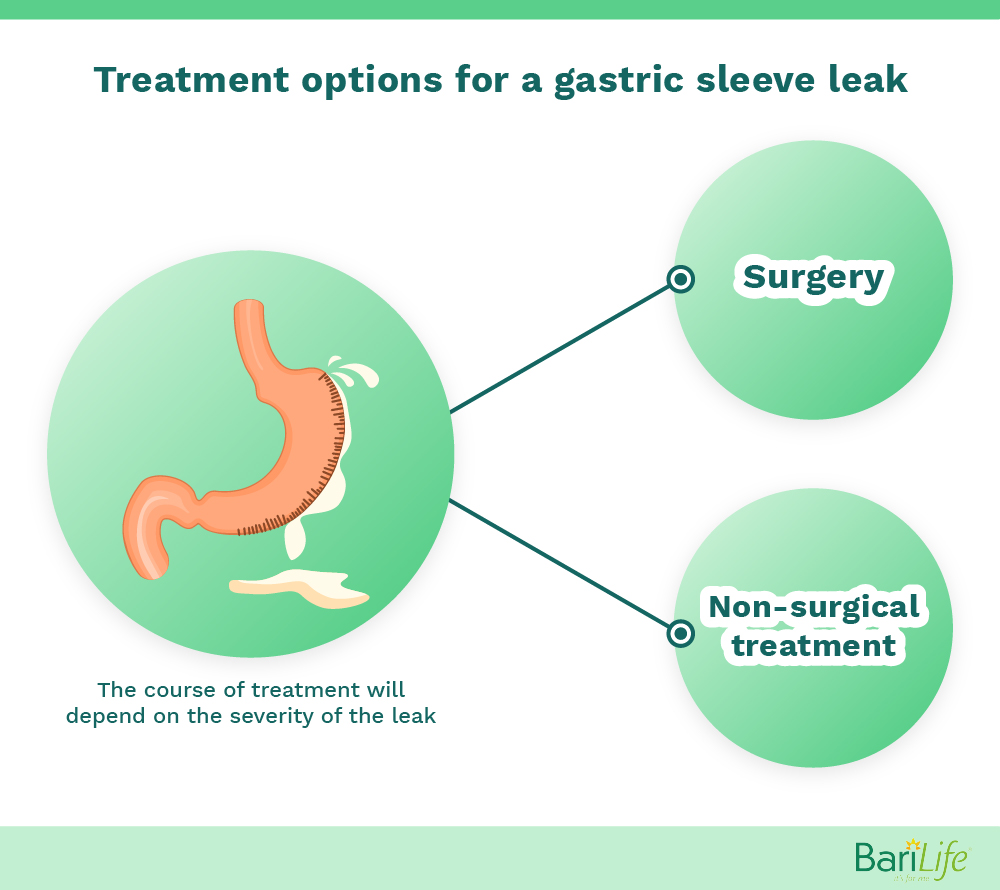
Nonsurgical treatments include being kept NPO (not being able to eat anything by mouth) and being provided hydration/nutrition through your veins, drainage of fluid, and/or a course of antibiotics.
What about surgical options?
If your gastric leak is severe, you may need to be treated surgically. The ASMBS notes that surgical options can differ between acute leaks, which have been ongoing for less than 5 days, and chronic leaks, which are present beyond 4 weeks.
In an acute leak, the main goal of surgery is to drain the fluid that is leaking, in order to avoid an infection. The surgeon may also insert a jejunostomy tube, which is a feeding tube that is located in the small intestine, in order to feed the patient and allow their stomach to rest.
If the leak is chronic, it will be more difficult to definitively seal surgically. Therefore, the ASMBS recommends nonoperative management in chronic fistulas rather than surgical management. Some surgical management techniques for chronic leaks that have been reported are conversion to a gastric bypass or total gastrectomy (complete removal of the stomach).
In summary: gastric leaks after sleeve gastrectomy
Between 1-3% of patients who have an LSG wind up with a gastric leak. After you have your LSG, it’s important to monitor yourself for symptoms of a leak, including an increased heart rate, fever, and/or rapid breathing. If you’re having any of these symptoms, it’s important to get in contact with your doctor as soon as possible for further evaluation.
This is especially crucial if you’re having a revision surgery, where leaks become much more common. If you’re concerned about the possibility of having a gastric leak, it’s important to discuss this with your physician prior to your surgery to discuss your options.


What are your tips and tricks to post-bariatric success?