Obesity is associated with the leading causes of death worldwide, including diabetes, heart disease, stroke, and some types of cancer. Weight-loss surgery can be a great option for those struggling with morbid obesity and experience obesity-related complications. Weight-loss surgery, including both gastric sleeve and lap band operations, achieves weight loss in patients by altering the gastrointestinal system.
According to the National Health Service of the UK, the different bariatric surgery techniques include making the stomach smaller to limit how much you eat and drink, while others change the small intestine so the body absorbs fewer calories from food. In order to qualify for weight loss surgery, there are certain criteria you must meet.
According to the American Society for Metabolic and Bariatric Surgery, to be considered a good candidate for weight loss surgery, you must meet the following:
- BMI ≥ 40, or more than 100 pounds overweight
- BMI ≥ 35 and at least one or more obesity-related co-morbidities such as type II diabetes (T2DM), hypertension, sleep apnea, and other respiratory disorders, non-alcoholic fatty liver disease, osteoarthritis, lipid abnormalities, gastrointestinal disorders, or heart disease
- Inability to achieve a healthy weight loss sustained for a period of time with prior weight loss efforts

Gastric sleeve surgery
Gastric sleeve is one of the main surgical techniques of weight-loss surgery. According to UCLA Health, this method involves removing about 75-80% of the stomach. The gastric sleeve surgery works by reducing stomach volume, causing people to feel full faster, thus eating less, hormonal changes causing people to feel less hungry, and increases stomach motility, which makes food pass the stomach and intestine faster.
Lap-band surgery
Lap band surgery, also known as laparoscopic adjustable gastric banding (LAGB), is another common surgical technique used for weight loss surgery. This procedure is a minimally invasive, quick, reversible, and adjustable surgical procedure that decreases the size of the stomach to reduce food intake. According to Columbia University Irving Medical Center, it involves placing a soft silicone ring with an expandable balloon in the center, around the top part of the stomach this results in a person feeling fuller with less food.
Gastric sleeve vs. lap-band weight loss
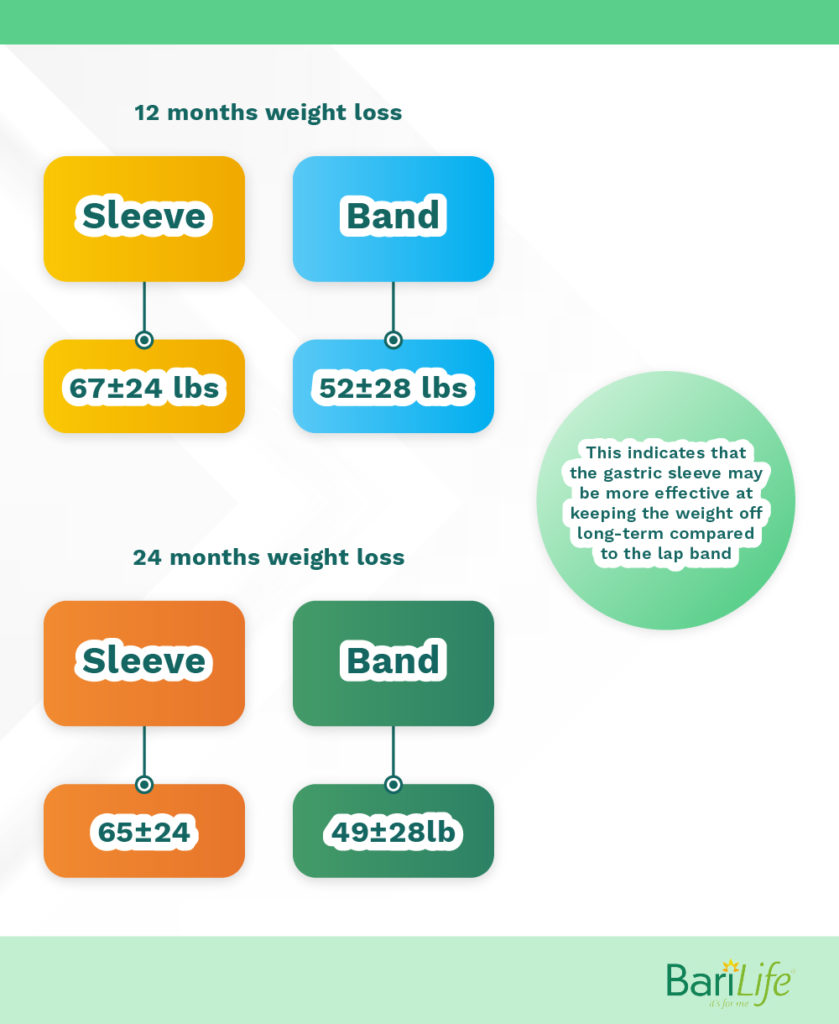
Both the gastric sleeve and lap band are effective techniques that can significantly reduce BMI after surgery. According to a study comparing the gastric sleeve with the lap band in high-risk patients, the total weight loss between both groups at 12 months was 67±24 lbs for the sleeve and 52±28 lbs with the band. However, at 24 months total weight loss was higher in the gastric sleeve group at 65±24 vs. 49±28lb with the lap band. This indicates that the gastric sleeve may be more effective at keeping the weight off long-term compared to the lap band.
Gastric sleeve vs. lap-band cost
According to Bariatric Journal, in the United States, an average gastric sleeve surgery typically ranges from $4,000 – $18,000. The lap band surgery falls into a similar price range and typically costs about $10,000 – $20,000.

Depending on the type of insurance you have, you may be eligible for partial or full coverage. The base requirements most insurance companies may require are proof that the surgery is medically necessary, previous attempts in weight loss programs, and a psychological and nutritional evaluation.
Gastric sleeve vs. lap-band complications
The gastric sleeve and lap band are considered much less invasive and lead to fewer complications compared to other weight-loss surgery techniques such as the Roux-Y gastric bypass. Similar to any major surgery, bariatric surgeries can pose potential health risks.
According to an article comparing potential complications of different bariatric surgery techniques in the Gastroenterology & Hepatology journal, some potential risks of gastric sleeve surgery include the following:
- Excessive bleeding from the long gastric staple line
- Leaks from the cut edge of the stomach
- Gastrointestinal obstruction: A blockage that keeps food from passing through the intestines
- Hernias: Forms at the site of any surgical incision. This looks like a small bulge at the site of a surgical incision
- Nutritional deficiencies: The most common deficiencies are vitamin B12, iron, calcium, vitamin D, vitamin b1, and folic acid
- Dumping syndrome: Increases gastric motility meaning food moves rapidly into the small intestines
- Vomiting: This can be most likely caused by overeating
- GERD

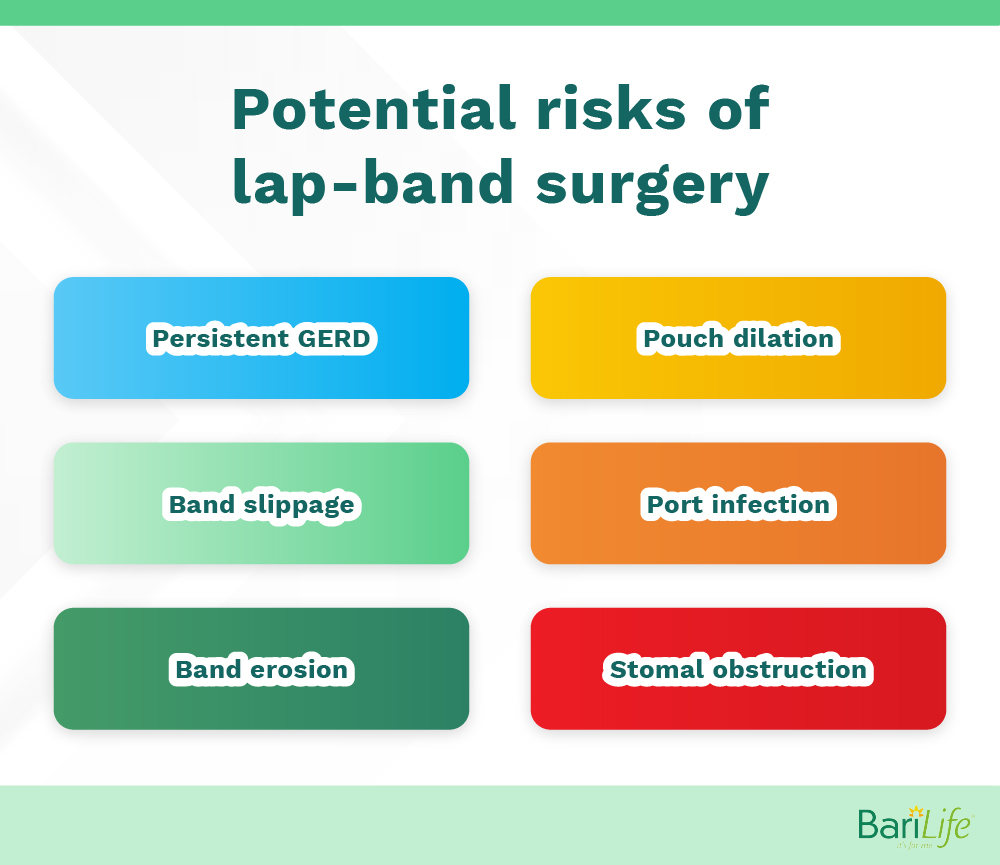
In the same article from the Gastroenterology & Hepatology journal, potential complications for gastric band surgery include:
- Persistent GERD: This is the most common symptom seen in patients after surgery. Behavioral diet modification and acid-suppressing medication can help to control symptoms
- Pouch dilation: The pouch enlarges due to high pressures on the pouch. This can be caused by overeating and may resent with GERD, and vomiting
- Band slippage: Involves migration of the band from its appropriate position, causing prolapse of the stomach above or below the band
- Port infection: Infection will present with local tenderness, warmth, and erythema
- Band erosion: Band erosion can be a serious complication that results in weight gain, abdominal pain, dysphagia, hematemesis, or sepsis
- Stomal obstruction: the flow of food from the gastric pouch to the rest of the stomach is blocked
Both procedures have low short-term minor morbidity and readmission rates with no associated major morbidity, reoperations, or mortality. Complication rates for both the sleeve and gastric band are at 13% of patients, according to an article from 2015, but the gastric band has a higher long-term reoperation rate, meaning that in the long run, the gastric sleeve may be the better option. Ultimately, it is up to you and your doctor to weigh the benefits and risks of each procedure to make a final decision.
Post Bariatric Surgery Diet:
After undergoing bariatric surgery, it is critical to follow the recommended guidelines provided by your healthcare provider. These guidelines ensure you are limiting the number of calories you consume but also eating balanced meals that help your body properly heal post-operation.
5 eating tips post-operation:
- Eat balanced meals with small portions
- Keep a record of your calorie and protein intake
- Eat slowly and thoroughly chew your food
- Do not use straws or drink carbonated drinks. This can lead to air coming into the pouch
- Sip 1 cup of water between meals

Key takeaways
Gastric sleeve and lap band surgeries are two of the main types of weight-loss surgeries. Gastric sleeve involves removing the majority of the stomach to help patients lose weight. Lap band surgeries, however, are minimally invasive and reversible. Lap band surgeries shrink the size of the stomach temporarily, allowing for adjustment and reversal. With both surgeries, serious complications can arise.




What are your tips and tricks to post-bariatric success?