If you are planning to have the gastric sleeve procedure it is important to be aware of the necessary lifestyle modifications and adjustments that you are required to make following surgery.
Knowing what to expect after the procedure can help you to optimize your recovery and weight loss. This article will provide an inside look at the first 3 months following the gastric sleeve procedure.
In this article, we will discuss postoperative management and recovery, physical activity, wound care, weight loss, diet, and fluid intake.
Post-op management and recovery for gastric sleeve
Immediately following surgery
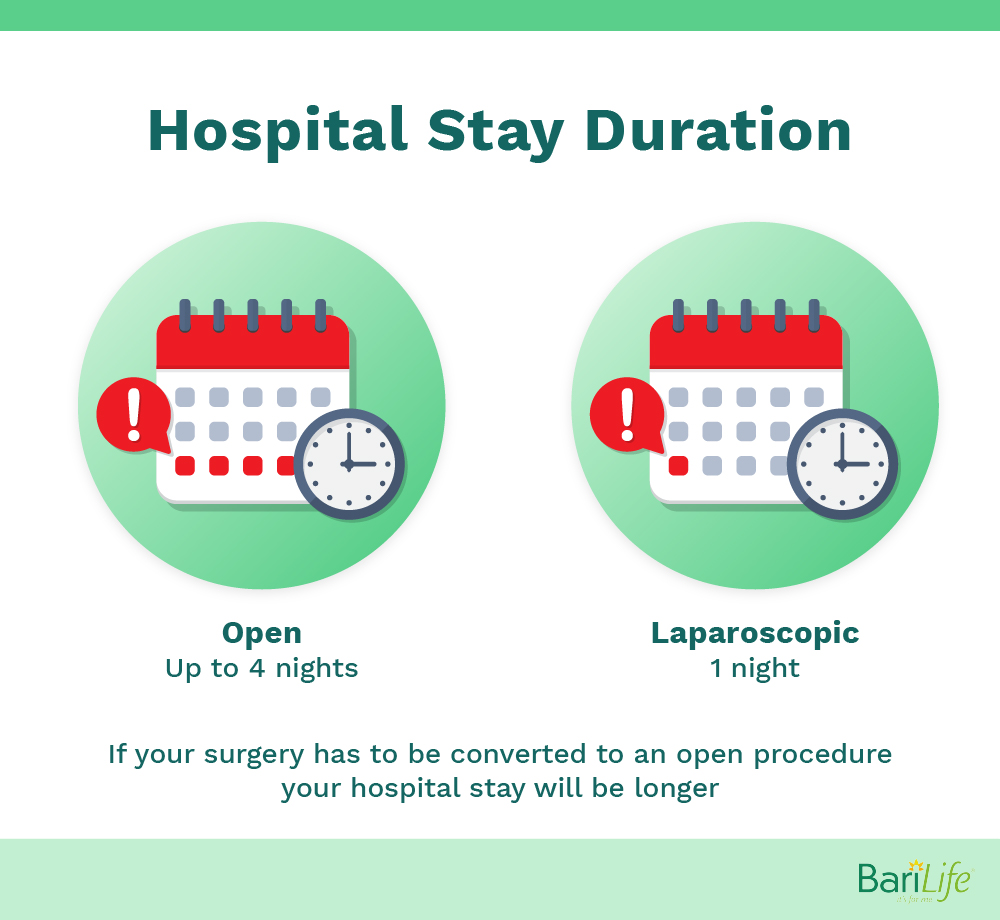
A study published by obesity surgery suggests that if you have an open sleeve gastrectomy your hospital stay will be around 2-4 days following surgery. If you have a laparoscopic sleeve gastrectomy you will likely have a shorter hospital stay. If you experience complications your hospital stay may need to be extended..
In your hospital room following the procedure you can expect to be monitored by a team of nurses and other healthcare providers.
In order to be discharged your healthcare team will be looking for you to…
- Tolerate an oral diet and fluid intake
- Not require the use of IV drugs or fluids
- Have balanced diuresis (proper urine output)
- Be able to manage your pain level with oral pain killers
- Be fever free
- Have properly healing surgical wounds
- Have a physical activity level similar to pre-surgery
- Be free from any complications
- Have someone to be able to help you at home the first few days
- Have a way to return to the hospital should complications arise

To enhance your recovery in the hospital you will be encouraged to perform deep breathing exercises, coughing, leg movement, and to get up out of bed. These exercises and movements can help to remove excess CO2 from the abdomen following laparoscopic surgery and enhance circulation which will promote a speedy recovery.
Symptoms you might experience shortly after surgery may include:
- Fatigue
- Nausea and vomiting
- Sleeplessness
- Surgical pain
- Weakness
- Poor appetite
- Gas pain and/or flatulence
- Loose stools
- Emotional ups and downs
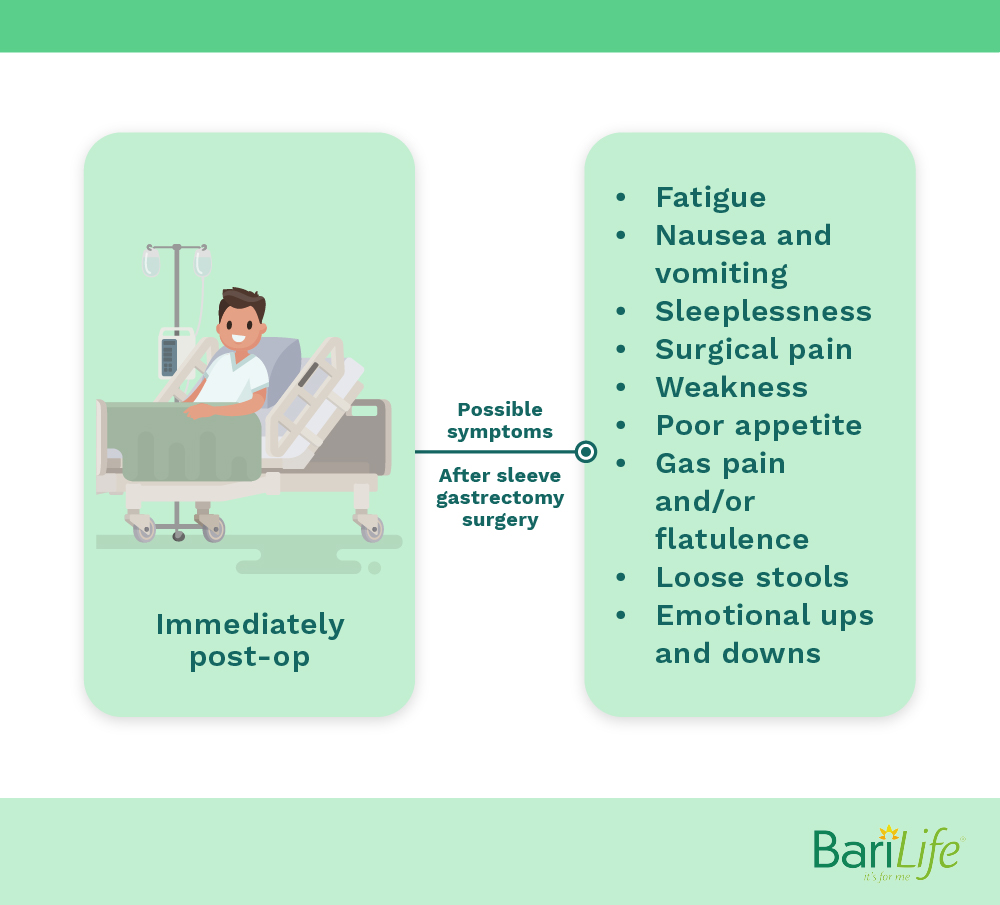
Concerning symptoms may include, but are not limited to, nausea, anxiety, muscle spasms, increased pain or shortness of breath. Be sure to communicate any of these concerning symptoms to your nurse or physician.
Pain management
Pain management is important following surgery. You may experience pain for a variety of reasons. Pain at the incision site, pain while resting in different positions, abdominal pain, and shoulder pain are not uncommon. Also, you may experience pain while moving or walking around following the procedure. It is important to manage your pain to a level that allows you to participate in the necessary rehabilitation activities.
Tips for pain management:
- Communicate to physicians or nurses if you are experiencing persistent or severe pain
- Plan ahead for pain – even if you are comfortable laying down, you may experience pain while moving around or during physical activity
Activity
Immediately following surgery, light movement and walking are highly encouraged. Post-operative movement and exercise can help to promote circulation, discourage the formation of blood clots, and enhance healing.
Initial exercises to maximize recovery:
- Walking
- Changing positions in bed
- Standing up
- Post-operative exercises
For the first few weeks after surgery, activity is encouraged within limits. You may experience weakness or fatigue after activity, so it’s better to keep activity short and frequent. A great example of this is short frequent walks. You can gradually increase the duration and frequency of your walks as you recover and based on how your body feels.
In the first two months following surgery, you can work towards a goal of 30 min of walking per day 5 times per week.
As you progress in your recovery, more physical activity is encouraged. The more physically active you are the better. Physical activity can promote a faster recovery and help you to have more energy. Better weight loss outcomes are also associated with increased physical activity.
Here is a guide to physical activity following surgery.
Physical activity to avoid post-op
It is very important to AVOID all strenuous activity for the first 3-6 weeks following surgery. This includes…
- Lifting anything weighing more than 20-30 lb
- Activity involving push-pull motions (ex. Vacuuming)

Do not lift, carry, or push heavy loads for the first 3 months following surgery and avoid sitting or standing for long periods of time without moving.
Wound care after gastric sleeve
A research study published by Obesity Surgery, suggests an overall surgical site infection rate of 1.4% following bariatric surgery. In this study 28 of the 2,012 participants experience an infection of their surgical incision site. This study showed a higher infection rate with laparoscopic bariatric surgery when compared to open bariatric surgery. If your surgical incision site becomes infected you may need to have an abdominal drain placed or a second abdominal operation.
How to care for your surgical incision site
Tending to your surgical incision site following surgery should require relatively minimal care. If sutures were used to close your incision site, they will likely dissolve and not need to be removed. “Steri-strips” or clear strips of tape may be used on the incision site as well. These strips should fall off on their own. If staples were used to close the wound, they will need to be removed. This usually occurs around day 10 following surgery.
It is important to keep your surgical wound clean and dry.
Try to let your incision site stay open to the air as much as possible. If the incision site is bothered by clothing or is oozing… then you may apply a light dressing to the wound, but try not to keep the dressing on longer than you need to. Leaving the wound open to the air can help to prevent infection.
After surgery, you may shower, unless stated otherwise by your physician. Gently wash with soap, rinse, and dry thoroughly. At about 3 weeks post-op it is generally okay to get your surgical incision completely wet. Make sure to get approval from your physician before fully submerging your surgical incision in water, i.e. taking a bath or swimming.
Signs your surgical incision might be infected:
- Redness or swelling
- Warmth at the incision site
- Red streaks
- Pus, Yellow/green, or odorous drainage
- Increasing soreness
- Fever above 100.5℉
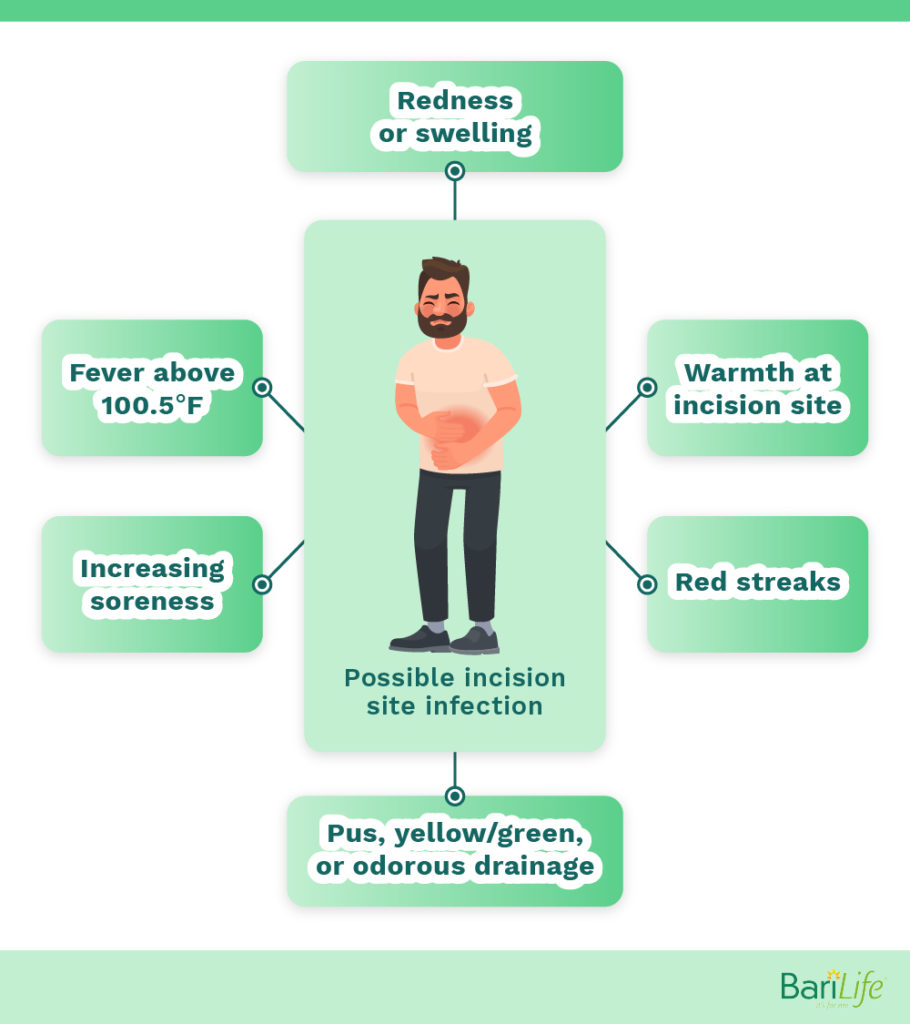
Research suggests that most surgical incision site infections occur within the first 2-3 weeks following surgery. Make sure to properly care for your surgical wound and If you experience any of these signs or symptoms, contact your surgeon right away. Do not try to treat the infected wound by yourself. Only use medications or ointments as directed by your physician.
Weight loss & Resolution of comorbidities
The sleeve gastrectomy can provide satisfactory weight loss in both obese and morbidly obese patients. A study published by obesity surgery found an average weight loss of 21 kg (~46lb) in the first 3 months following the gastric sleeve. The percent of excess weight lost by participants in the first 3 months of this study was 33.1%. At the start of this study, the average BMI was 43.2kg/m2 and after the first 3 months, the average BMI was 36.9 kg/m2, meaning the average drop in BMI was 6.3 kg/m2.
On average the highest percentage of weight loss occurs in the first 3 months of surgery.
This study evaluated the association between weight loss and changes in BMI at 3 months and long-term weight loss at 2 years. The findings suggest that weight loss or changes in BMI at 3 months can be a strong strong predictor of long-term success.
This means that if you are not seeing good results 3 months post-op, you may want to follow-up with your team of bariatric healthcare professionals. A multidisciplinary approach can help you to achieve the results you are looking for.
Both Nutrition and physical activity are factors that impact both short and long-term weight loss.

Here are some reasons why you might not be losing weight after the gastric sleeve.
Diet and fluid intake after gastric sleeve
Diet
Following the gastric sleeve procedure, food will have to be reintroduced slowly. Your diet will progress through a few phases in the first 3 months following surgery.
The 4 phase diet approach:
Phase 1 – LIQUID PROTEIN DIET – First 2 to 4 weeks
Phase 2 – PUREED DIET – The next 2 to 4 weeks
Phase 3 – SOFT FOOD DIET – The following 8 weeks
Phase 4 – STABILIZATION DIET- Initiated around 4-6 months after surgery and continued for life
Fluid intake
Fluid intake is one of the most important factors following bariatric surgery. Inadequate fluid intake can be associated with longer postoperative hospital stays or readmission to the hospital due to dehydration.
It is recommended that you drink 1.5-2 L of water per day.

If you are struggling with fluid intake due to nausea or vomiting, it is encouraged that you take small frequent sips of water.
In summary…
The sleeve gastrectomy can promote weight loss and improved quality of life, but the road to recovery and results isn’t always easy. Educating yourself on what to expect can help you to have a better surgical experience and recovery.
Communication with healthcare providers is vital when you are experiencing concerning symptoms or if you aren’t achieving your desired results. Early activity and movement, adequate fluid intake, and adherence to diet are vital factors in weight loss and recovery.
Bariatric surgery requires lifelong changes in diet and lifestyle. Adequate recovery and lifestyle modifications in the first 3 months can set you on the right track to achieving the long-term results you are looking for.




What are your tips and tricks to post-bariatric success?